What is Fuchs' Corneal Dystropy?
Fuchs' corneal dystrophy (FCD), or Fuchs' endothelial dystrophy, is a serious condition affecting the cornea, or lens of the eye, and most commonly affects older adults
The innermost cells of the cornea, called the endothelium, begin to degenerate. This tissue is normally responsible for regulating fluid within the cornea, as too much or too little fluid can negatively affect vision. Typically both eyes are affected simultaneously, and vision will gradually become cloudier as the disease progresses. The cornea may also swell and blister, leading to bullous keratopathy.
Some cases of FCD are hereditary, being passed from generation to generation. Just one parent having FCD results in a 50% chance of their child developing the disease later in life. However, some people can develop the disease without any family history at all. In these cases, the root cause of the disease is not currently known. It is most commonly found in people who are middle-aged or older, but it can develop in younger people and affects women more often than men.
Signs and Symptoms of Fuchs' Corneal Dystrophy
Symptoms of FCD can develop slowly, or quickly, and not all those affected will exhibit the same symptoms.
A classic symptom of Fuchs' Corneal dystrophy is "morning misting" - this is where the vision appears misty or cloudy when you wake up but clears as the day progresses.
Some other of the symptoms that may appear include:
- The appearance of light glare
- Sensitivity to light
- Pain or discomfort in the eye
- Blurry vision
- The appearance of halos around lights
- Poor night vision
- Poor morning vision that improves throughout the day
- Foreign body sensation
If any of these symptoms are experienced, it's strongly recommended to schedule a comprehensive eye exam with an eye care professional. The exam will allow the optometrist to make a diagnosis, either of FCD, or any other potentially vision-threatening disorder, and prescribe the appropriate treatment.
To diagnose FCD specifically, a magnified image of the cornea is taken with a tool called a slit lamp, which allows the doctor to view all of its layers. The endothelium, the one affected by FCD, will be examined to determine the amount of fluid within.
One of the earliest signs of FCD is a lower than normal number of endothelial cells within the cornea. This alone is not enough to cause a noticeable change in vision, meaning that few people ever notice it on their own without a medical diagnosis. The next symptoms likely to develop are the thinning or thickening of the cornea and the growth of small lesions called guttata in the corneal endothelium. The thinning or thickening of the cornea is likely going to affect visual acuity, providing the first noticeable symptom that brings people to their eye doctor.
What are Epithelial Bullae?
Epithelial bullae can be a symptom of Fuchs' corneal dystrophy and are small blister-like lesions, that develop on the eye, they continue to grow and eventually rupture, releasing the fluid contained within them onto the surface of the eye, which can be painful and disrupt vision. This is known as it is known as bullous keratopathy.
These blister-like lesions can cause increased sensitivity to light, halos around lights, and increased glare, they can also cause your eyes to water.
Treatment for Fuchs' Corneal Dystrophy
While there are currently no prevention methods for FCD, it is possible for it to be treated. The method of treatment will entirely depend on its stage of development. In the early stages, vision can often be improved by removing excess water from the cornea with 5% sodium chloride (hypertonic) eye drops. If you have endothelial dystrophy and raised interocular pressure, glaucoma eye drops may be prescribed to help reduce the internal eye pressure.
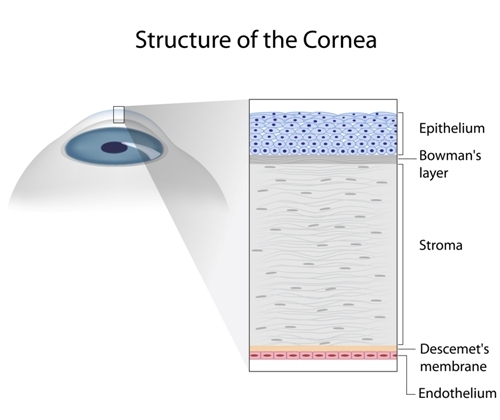
If epithelial bullae have already developed, unfortunately, the damage is irreversible, and can only be fixed with a complete corneal transplant (penetrating keratoplasty or PK) or deep anterior lamellar keratoplasty (DALK), which is a surgical method to replace the endothelium that leaves the upper layers of the cornea untouched. This procedure has shown to be successful for the treatment of Fuchs' dystrophy with potentially fewer risks than penetrating keratoplasty.
In recent years, an advanced form of DLEK called femtosecond laser-assisted Descemet stripping endothelial keratoplasty (FS-DSEK) has shown encouraging results for the treatment of the disease.
Fortunately for most FCD sufferers, it is a slow developing condition, and it is possible these symptoms will take a long time to develop.
Quick note: FCD sufferers should avoid LASIK or other forms of refractive surgery. These eye surgeries are likely to exacerbate the condition, most refractive surgeons won't operate on anyone that has been diagnosed with the disease.

