What Is Uveitis?
You have probably not heard of Uveitis but recent estimates from Moorfields Eye Hospital found that about 4 in every 10,000 people in the UK are diagnosed with uveitis annually. Even more concerning, doctors claim uveitis puts patients at a greater risk for developing visual impairment later in life. Despite these alarming figures, most eye care patients in the UK don’t know much about this chronic condition.
So, what is this visual disorder and how could it cause such severe damage to a person’s eyes? In this piece, we’ll explore the most pertinent questions surrounding uveitis. This article will also explore strategies everyone can put into place to minimize the risk of developing uveitis.
What Is The Uvea?
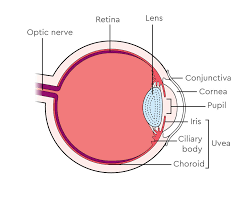
Whenever you see the suffix “–itis,” most people instantly think of “inflammation.” Conveniently, the prefix in most “–itis” illnesses tells us exactly which part of the body is inflamed. So, in the case of uveitis, we have to focus on an area of the eye known as the Uvea.
Basically, the uvea refers to a thin layer in the middle of the eye that’s composed of three tissues. Of these three tissues, the most well-known is the iris. this is the circle around the pupil that gives your eye its colour. In addition to colouring your eyes, the iris plays a supporting role in focusing the pupil.
The other two areas in the uvea are known as the ciliary body and the choroid. The main duty of the ciliary body is to help stabilize the lens. The choroid, on the other hand, helps supply nutrient-rich blood to the retina.
The Different Forms Of Uveitis
As we’ve just discussed, the word “uveitis” refers to inflammation in the uvea. This term, however, doesn’t tell us exactly which tissues are inflamed in the eye.
Over the years, doctors have observed a few different varieties of uveitis, each of which affects different tissues in the uvea. For instance, some patients only have inflammation in the ciliary body (aka intermediate uveitis) while others have inflammation in all three uveal tissues (aka diffuse uveitis). It’s important for sufferers to understand exactly what form of uveitis they have so they know the best way to treat their disorder.
Today, doctors split uveitis into four major categories:
- Anterior - Inflammation in both the iris and ciliary body
- Intermediate - Inflammation in the ciliary body.
- Posterior - Inflammation in the choroid
- Diffuse - Inflammation in all three of the uvea’s tissues
Sometimes anterior uveitis can get confused with another disorder called iritis. The only difference between these similar conditions is that people with iritis only have inflammation in the iris. There are a few doctors who consider iritis to be in its own category, but technically it’s also a form of uveitis.
What Are The Warning Signs And Symptoms Of Uveitis?
Unfortunately, uveitis usually doesn’t present any obvious warning signs until it has progressed a great deal. Many of the visual symptoms of uveitis can easily be mistaken for benign conditions like dry eye syndrome.
A few common warning signs of uveitis include
- Photophobia
- Increased tearing
- Eye redness
- Eye floaters
- Eye pain
- Temporary blurred vision. If you're wondering how long blurred vision lasts with Uveitis this could last for a few weeks.
If you experience eye pain due to uveitis, then you most likely have either the anterior or diffuse form of the disorder.
People with untreated uveitis have a greater chance of developing many potentially blinding conditions like glaucoma and cataracts than non-uveitis sufferers. Anyone is at risk of developing uveitis, but particularly so for people in their 20s - 60s, regular eye screening can help detect uveitis before it becomes too developed. The earlier doctors treat uveitis, the better chance you have of preserving your sight for the rest of your life.
What Causes Uveitis?
It can not always be determined what causes some cases of Uveitis, however, doctors do recognise several risk factors
- Direct trauma to the eyes
- Smoking
- Auto-immune diseases
It is thought, a uveitis sufferer’s immune system mistakenly perceives healthy uveal cells as invaders and attacks them. Doctors who support this theory note that a majority of uveitis patients have other immune-related disorders like Lupus, Rheumatoid Arthritis, Lyme disease and ulcerative colitis. Meaning, uveitis could potentially be considered an autoimmune disorder or a complication of other autoimmune conditions.
It’s important to remember that the science of the connection between uveitis and autoimmunity is only in its initial phases. Still, this research offers great hope for the future treatment of uveitis.
Uveitis Treatment Options
While there’s no cure for uveitis, doctors can help patients manage their uveitis with various medications and surgeries. Keeping uveitis-related inflammation in check is critical for avoiding more serious visual complications later on.
The treatments your doctor decides to use will depend on what type of uveitis you have. If you have an underlying autoimmune condition, then your doctor will suggest treatments for that as well.
To help with eye inflammation, your eye doctor will most likely prescribe corticosteroid and/or immunosuppressant medication. For those with a more severe case of this disorder, you might have to get regular eye injections. Surgery on the vitreous humor is only recommended for extreme cases of uveitis.
How To Prevent Uveitis
While there are many treatments now available that can help manage uveitis, it’s always better to avoid having to contend with this condition in the first place. Thankfully, there are many simple steps everyone could take to dramatically lower their risk of developing uveitis. Below, we’ll share a few powerful strategies that could massively improve your eye health.
Quit Smoking
Smoking is the number one preventable cause of uveitis. Researchers at the American Academy of Ophthalmology say smokers also have a higher risk of developing other eye disorders such as cataracts and age-related macular degeneration compared with non-smokers.
To help UK smokers quit this harmful habit, the NHS has set up a “Smokefree” program that’s full of helpful resources. For more information on “Smokefree,” be sure to talk with your primary care physician or visit this official portal.
UV Protection
In 2017, a group of Taiwanese researchers analyzed the effects of ultraviolet (UV) rays on the eyes of a group of mice. They found that mice who were exposed to high levels of UV rays had the greatest chance of developing uveitis. By contrast, mice who wore contact lenses with UV protection had significantly lower eye inflammation.
This study clearly shows prolonged exposure to UV rays has a deleterious effect on the uvea. Whether you have uveitis or not, it’s always a wise idea to wear UV-blocking sunglasses when you’re outside. If sunglasses don’t work for your lifestyle, then consider ordering a pair of glasses or contacts with Transitions technology.
A Feast For The Eyes: Diet Tips For Uveitis Sufferers
A recently published meta-analysis out of China highlighted the importance of eating an antioxidant-rich diet for maintaining healthy eyes. In particular, researchers looked for correlations between people’s diets and their risk for cataracts. Unsurprisingly, people who had a diet full of antioxidant-rich fruits and veggies had the lowest risk of developing cataracts later in life.
While there’s no meta-analysis specifically analyzing the effects of diet on uveitis risk, it is known that eating more fresh fruits and veggies can help your overall eye health. Dark, leafy greens like spinach, kale, and Swiss chard are particularly good for eye health because they have high amounts of lutein and zeaxanthin. Both of these compounds have been shown to reduce eye inflammation and protect the retinae from damage.
Since uveitis is an inflammatory disorder, it’s also a great idea to include anti-inflammatory foods like ginger, turmeric, and cayenne pepper into your diet. Antioxidant-rich fruits like blueberries, cherries, and pomegranates are also great additions to any uveitis diet plan.
Nip Uveitis In The Bud: Get Your Eye Exam Today
You may not be able to prevent uveitis but by visiting an optometrist for regular visual screenings you can detect it early. Even if you don’t experience obvious symptoms of uveitis, that doesn’t mean the disease isn’t already present in your eyes. The NHS recommends all patients who have healthy vision and are under the age of 40 should get a vision check-up once every two years. For more info on how frequently you should see a UK optometrist and whether you qualify for a free sight test or prescription glasses or contact lenses, then check out the NHS website.
Don't forget, if you have any worries or concerns, speak to your optometrist, or you can check out our Eye Help pages, which are available to everyone, however, if you order lenses from us, you will have access to our contact lens aftercare pages, and our optometrist from within Your Account.

